Protecting Your Patient Rights
WakeMed is Out of Network for Commercial & Medicare Advantage Plans
Commercial contract negotiations continue in hopes of reaching an agreement.
At WakeMed, we never compromise when it comes to delivering high-quality patient care. In the interest of patients and our community, we negotiate insurance agreements in good faith and do not back down from the commitments we make. In return, we only ask that insurers honor their side of those agreements.
For over a year, WakeMed has been working in good faith with UnitedHealthcare (UHC) to come to a contract agreement that ensures your continued in-network access to high-quality care and services with the WakeMed providers you know and trust. Unfortunately, we have so far been unable to reach an agreement.
As a result, WakeMed hospitals, outpatient facilities and physician specialists are now considered out of network for UHC. This change impacts out-of-pocket costs for most patients with UHC insurance. If you have an upcoming appointment at WakeMed, please review your options and next steps.
Please note that WakeMed primary care physicians are not included in these current negotiations and will remain in network. Patients with UHC insurance may continue to see their primary care physicians with no change to services or costs.
If You Need Emergency Care
Please be aware that all patients, regardless of their insurance status, may still seek treatment at any of WakeMed’s eight Emergency Departments, including the county’s only Children’s Emergency Department.
Under the No Surprises Act, emergency services must be covered by the patient’s insurer without prior authorization, regardless of whether the facility/provider is in-network or out-of-network, and without regard to any other term or condition of the patient’s insurance plan or coverage.
This means that patients will pay the same amount for emergency care and post-stabilization services (including inpatient admission from the Emergency Department, if needed) as they would if WakeMed were in-network with their insurance plan. Patients do not need to transfer to an in-network facility once the emergency medical condition is stabilized to benefit from the financial protections of the No Surprises Act.
Where Negotiations Stand Currently
WakeMed remains committed to reaching a fair and sustainable agreement with UnitedHealthcare (UHC) that restores and preserves patient access to high quality, cost effective care for the communities we serve.
WakeMed submitted comprehensive commercial reimbursement proposals to UHC in late March that are intended to address longstanding, documented reimbursement disparities and align reimbursement rates more closely with what UHC already pays comparable high acuity providers in the Triangle.
In early April, UHC responded but would not discuss the documented reimbursement disparities that WakeMed provided, which are based on UHC’s publicly reported data. Instead, UHC stated that if WakeMed would not reconsider its March proposal and submit a new proposal, then the parties are not aligned and should end the discussions. WakeMed has advised UHC that this data cannot be ignored and is critical to any contract agreement. At this time, it is unclear if UHC has ended negotiations with WakeMed. We have asked UHC to respond clearly regarding their intent and notify WakeMed, their members and stakeholders accordingly. It is a disservice to our patients to publicly state that negotiations are continuing if they – in fact – are not. In response, WakeMed has proposed some options for UHC to consider, however we will not withdraw our prior proposal which requires UHC to acknowledge the market reimbursement disparities they alone have created.
For many years, UHC has reimbursed WakeMed at levels that are significantly below what it pays other health systems in our region for the same services. WakeMed has historically accepted lower reimbursement levels relative to peers, which has contributed to affordability in the market, but this gap has widened to an unsustainable level that must now be corrected.
WakeMed was founded by this community 65 years ago with a commitment to provide outstanding and compassionate care to all. As a not-for-profit hospital system, reasonable agreements with health insurance companies that allow us to be compensated for the true cost of care are crucial to our ability to serve as Wake County’s only children’s hospital, Level IV NICU, and state-designated Trauma Centers, among our many other services.
WakeMed remains ready to continue negotiations; however, progress requires meaningful engagement from UHC on addressing these longstanding reimbursement disparities.
UHC Data Reflects Consistent Rate Disparity
UHC’s publicly reported data (as of November 2025) demonstrates that WakeMed is paid considerably less than comparable hospitals and specialty physicians across a broad range of services. For purposes of this comparison, WakeMed is compared to Triangle-area hospitals with a state-designated Trauma Center).
The data below represents just a small sample of this longstanding pattern. These comparisons are based on UHC’s own publicly reported, machine-readable pricing data and reflect consistent patterns across a broad set of services.
It is also important to note that WakeMed’s proposals are not intended to achieve immediate parity with other systems, but rather to incrementally close a well-documented reimbursement gap and move toward reasonable market alignment over time. Even with these adjustments, WakeMed’s rates would remain below those of comparable high-acuity providers in the Triangle.
Hospital-Based Services
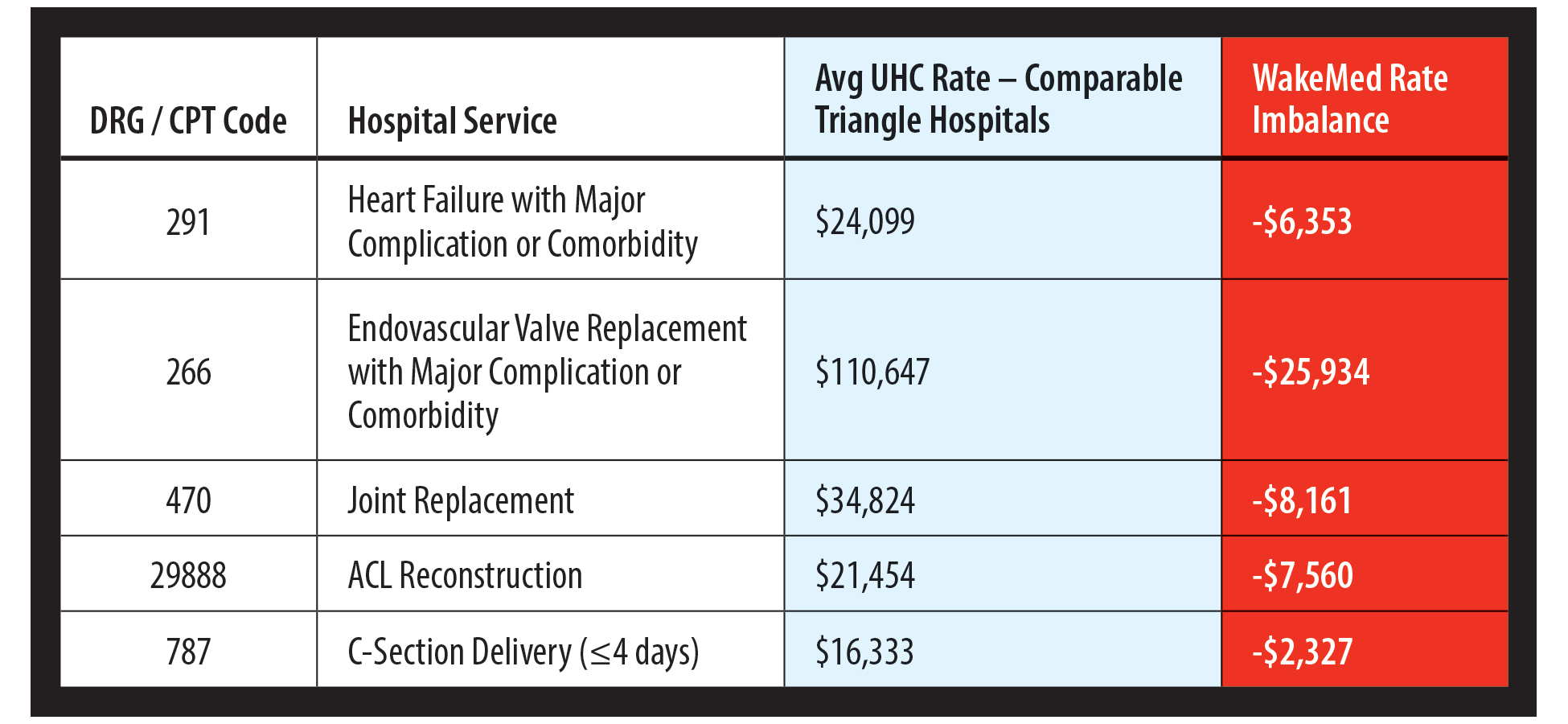
Physician Services
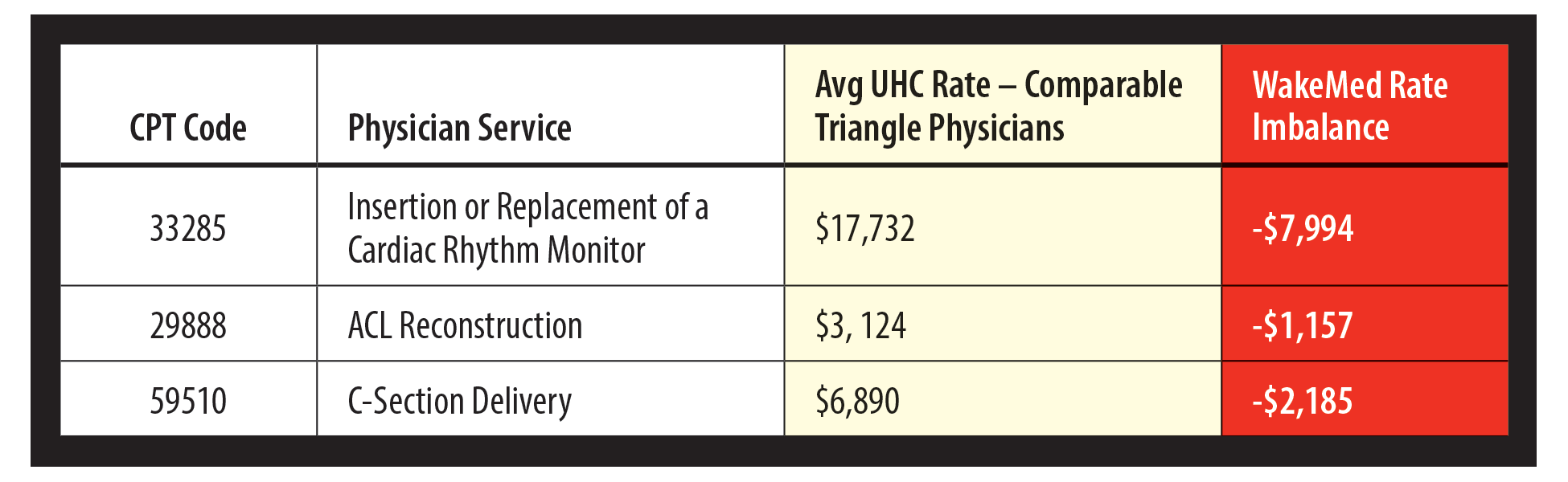
Despite what UHC may state publicly, WakeMed’s latest proposals are consistent with market benchmarks and the realities of delivering high-quality health care in a rapidly changing industry. We remain committed to a fair resolution that supports patient access and sustainability.
How You Can Help
If you want to continue receiving in-network care from WakeMed, help us negotiate on your behalf by:
- Calling UnitedHealthcare at the number on the back of your health insurance card. Ask UnitedHealthcare to reach a new agreement that maintains your in-network access to WakeMed and protects the relationship you have with your physician.
- If you have employer-sponsored health insurance, talking to your employer or HR representative about your desire to have continued access to WakeMed’s high-quality caregivers and services. You can also suggest your employer call WakeMed’s Managed Care Department at 919-350-7983.
We will continue to keep you updated on our negotiation progress. Rest assured; we are working hard to resolve this issue as we want to continue being able to serve your health care needs.
FAQs
As of November 15, 2025, all UnitedHealthcare commercial and Medicare Advantage insurance plans are out of network with WakeMed hospitals, outpatient facilities, urgent care and specialty care WakeMed Physician Practices.
Please note that WakeMed primary care physicians and MyCare365 locations are covered under a separate contract and are not impacted by these current negotiations. WakeMed’s retail pharmacies are covered under a separate contract and will remain in network for UnitedHealthcare members having Part D coverage.
The UnitedHealthcare Community Plan (Medicaid) is also excluded. However, UnitedHealthcare Medicare patients who have dual coverage with UnitedHealthcare Medicaid coverage will be impacted as UnitedHealthcare Medicare is your primary coverage.
Individuals covered under a UnitedHealthcare insurance product will likely see an increase in their out-of-pocket costs if they choose to receive non-emergency medical services at a WakeMed hospital, outpatient facility or at a specialty WakeMed Physician Practices location. Care will be considered out of network and out-of-pocket costs for most patients with UnitedHealthcare insurance will increase.
If you are a UnitedHealthcare Medicare Advantage plan member with an upcoming appointment, please visit this page to read more about your options and next steps.
Please note: all patients, regardless of their insurance status, may still seek treatment at any of WakeMed’s eight Emergency Departments, including the county’s only Children’s Emergency Department.
If you are covered under a UnitedHealthcare commercial insurance plan, you can call 919-350-8359 to speak with a member of our Patient Financial Services team.
It is also beneficial to speak directly with UnitedHealthcare to understand what they will cover when your care team is out of network. Ask what level of out-of-network benefits you have. Based on your individual plan, using an out-of-network provider or facility may lead to higher costs for you.
Throughout our negotiations, we have been focused on is about making sure that our patients get the benefits you are entitled to and that your care decisions are based on medical need—not corporate profit.
We’re asking UnitedHealthcare to agree to a contract that:
- Protects your relationship with your WakeMed physician
- Ensures access to medically necessary care
- Requires UnitedHealthcare to honor the terms of our agreement
Resolving these issues remains our priority and focus and has – to this point – precluded us from evaluating any comprehensive contract proposal. UnitedHealthcare’s most recent proposal offered no measurable increase in reimbursement rates for the next four years – despite expected increases in labor, supply and equipment costs.
Since 2016, hospital operating costs have climbed nearly 36 percent nationwide – and these trends continue. As a UnitedHealthcare employer and member, your costs for coverage have likely increased in recent years as well.
During the past nine years, our reimbursement rates with UnitedHealthcare have increased very modestly, and far below our cost increases. As a result, WakeMed is currently being reimbursed by UnitedHealthcare at 2019 levels, while WakeMed is paying 2025 costs for wages, supplies, pharmaceuticals, etc. Again, what they are charging you and your employer have certainly kept pace – and those additional revenues coupled with denials of medically necessary services are driving UnitedHealthcare’s record profit margins.
Unfortunately for sick patients across the country, these issues with UnitedHealthcare are not just a ‘WakeMed problem’. We are not the only health system asking UnitedHealthcare to honor their contractual agreements and ensure our patients’ covered benefits are not being denied.
Whether it is reporting record profits for the benefit of stockholders, U.S. Department of Justice investigations into UnitedHealthcare executives, denials of potentially life-saving care, or multiple health systems going out of network due to contract battles, the news is full of articles about ongoing issues and negative stories related to UnitedHealthcare. Time and again, UnitedHealthcare has put profit above the needs of their members – our patients.
UnitedHealthcare is trying to balance their margins on the backs of patients. This is the real reason health care costs are rising. In fact, UHC reported over $10 billion in earnings in the first two quarters of 2025 and $32.3 billion for calendar year 2024.
We understand that a potential network outage can be disruptive – and we want to assure you it is always our hope to resolve these issues without interrupting our patients’ care. At the same time, we must do all we can to ensure our contracts with insurance companies protect the relationships between our patients and their physicians, allows WakeMed to receive adequate reimbursement for services provided and supports our mission to care for all members of our community.
WakeMed accepts many other insurance plans, and this list is readily available on our website. We encourage patients to visit this web page to explore the other options we accept.
All of WakeMed’s hospitals, stand-alone emergency departments, urgent cares, outpatient services including imaging, laboratory, rehabilitation, wound care, sleep center, 210 PET and outpatient surgery centers are affected as are the WakeMed Physician Practices specialists.
WakeMed Primary Care practices and physicians, including MyCare 365, operate under a separate contract, which is not included in this negotiation. Additionally, WakeMed’s retail pharmacies will remain in network for UnitedHealthcare Part D members.
Updated April 8, 2026