Treatments
In this section:
- Thrombolytics (clot busting medication)/Thrombectomy (clot retrieval procedure)
- Angioplasty and Stenting
- Coiling/Clipping/Neurosurgical Care
- Primary and Secondary Prevention
- Stroke Vagus Nerve Stimulation Rehabilitation
- Acute Stroke Quality Metrics
At WakeMed, our Joint Commission-certified Thrombectomy-Capable Center team demonstrates skill and expertise, using the latest tools to reduce the length of stay and mortality in cases of stroke.
Thanks to dramatic advances in technology and the way strokes are treated, more Americans are surviving strokes and experiencing fewer permanent side effects than ever before.
Treatment Options
Once at the hospital, the patient will need to have blood tests as well as a computed tomography (CT) scan to determine if and where a clot exists.
These treatments include:
Ischemic Stroke Care
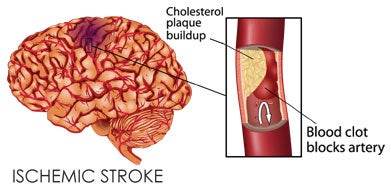
Thrombolytics (clot busting medication): Tenecteplase
- This medication is offered 24/7 for the emergent treatment of acute ischemic strokes.
- This medication is only used to treat stroke within 4.5 hours of stroke onset. Time is of the essence!
Thrombectomy: Procedure to Remove Clots
Intra-arterial mechanical thrombectomy is a minimally invasive procedure that, when performed in conjunction with Tenecteplase administration can remove clots and stop a stroke in its tracks. The results can minimize or completely eliminate the long-term side effects of stroke, such as speech, dexterity and mobility issues.
During the thrombectomy procedure, doctors use an innovative, catheter-based technology to capture the clot and pull it out of the artery, which restores blood flow to the brain. This procedure is performed using BiPlane technology, an advanced imaging system that helps guide instruments through the artery to the clot. WakeMed is a Value Partner with Siemens Healthineers, makers of the Artis Icono BiPlane technology used in thrombectomy procedures.
The procedure is performed 24/7 by neurointerventionalists in the cath labs at WakeMed Raleigh Campus and WakeMed Cary Hospital.
Permissive Hypertension
For patients who are unable to receive the clot busting medication or clot retrieval procedure, neurology providers may recommend allowing their blood pressure to remain elevated to better perfuse the brain for a brief period of time.
Angioplasty & Stenting
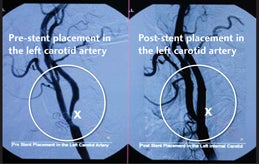
Angioplasty, a procedure commonly used to open blocked coronary arteries, is also an option to return blood flow to the brain for some stroke patients.
In this procedure, an interventionist threads a catheter containing a balloon to the site of the blocked carotid artery, and then inflates the balloon to open the artery.
The interventionist may also place a stent, a tiny device made of metal mesh, at the site of the blockage to help prevent future blockages that could cause strokes.
Learn more about WakeMed's vascular surgery options.
Hemorrhagic Stroke Care
Brain Bleed
- Aneurysm coiling/clipping
- Blood pressure control and blood thinner reversal
- These measures are taken immediately upon identification of a brain bleed to attempt prevention of increased bleeding.
- Neurosurgical services
Primary and Secondary Prevention
- Depending on your health history and brain imaging results, you may be prescribed medications to prevent a future stroke. If you are prescribed these medications, it is critical to fill the prescriptions and take them as ordered to reduce your risk of stroke.
- Here are example medications:
- Anticoagulants (blood thinners)
- Antiplatelets
- Antihypertensives (blood pressure medications)
- Statins
Stroke Vagus Nerve Stimulation (VNS) Rehabilitation
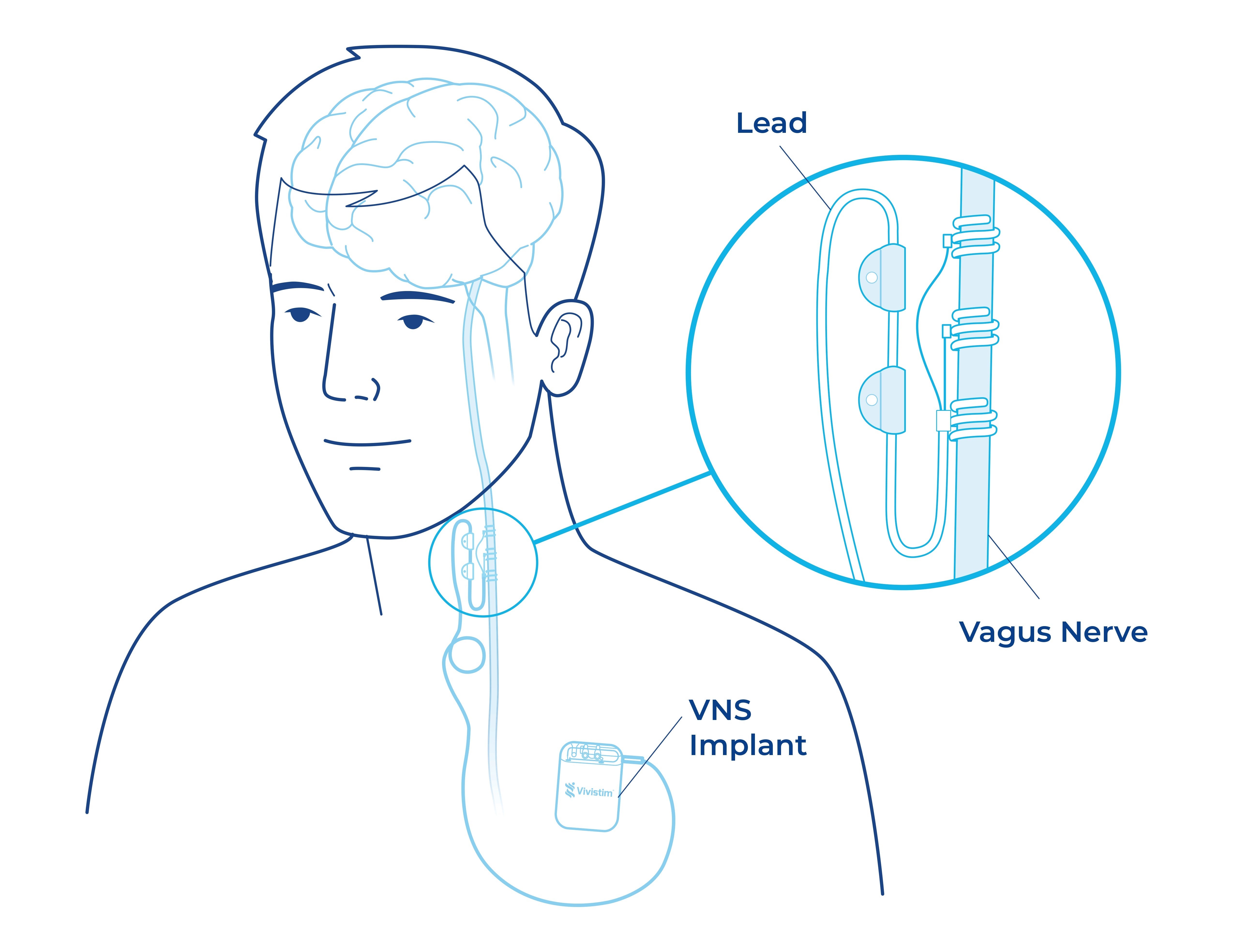
Stroke Vagus Nerve Stimulation (VNS) Rehab is an innovative therapy that pairs a small, implanted device with occupational therapy to help stroke survivors improve hand and arm function. By stimulating the brain through the vagus nerve, it helps create new neural pathways that support motor recovery — even years after a stroke. This combined approach can lead to significantly greater functional gains and improved independence compared to therapy alone.
Acute Stroke Quality Metrics
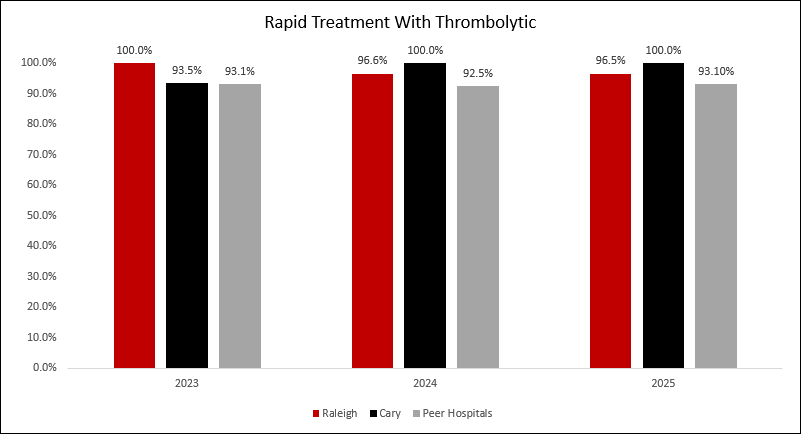
This chart shows the percentage of patients who arrive within two hours of their “Last Known Well”, or stroke symptom onset, and receive the clot busting medication within three hours of their Last Known Well. WakeMed consistently performs above Peer Hospitals nationwide.
The “Last Known Well” is a critical timeframe that the care team uses to determine stroke onset and treatment eligibility, as the clot busting medication (thrombolytic) can only be used within 4.5 hours of stroke onset.
In 2025, 79 percent of ischemic stroke patients who arrived to the hospital within 4.5 hours of stroke symptom onset and received Tenecteplase were able to either discharge home or to Inpatient Rehab.
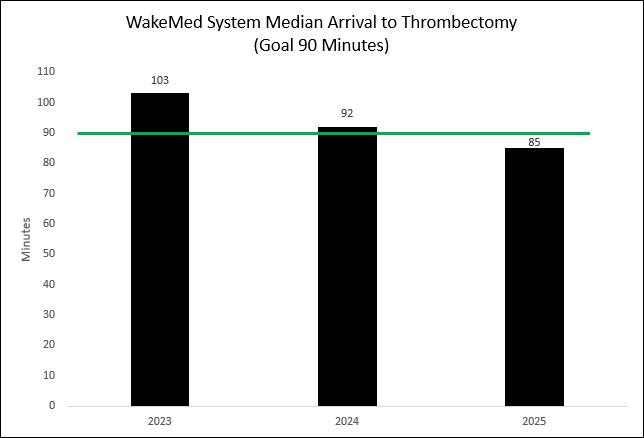
Every minute counts when it comes to stroke, and it is critical for our patients to have emergent access to treatment to save as much brain tissue as possible. The AHA recommends that patients arriving in the Emergency Department with stroke receive a thrombectomy within 90 minutes of their arrival time. WakeMed continues to improve our times and increase patient access to this care.
Patients with large strokes have historically required discharge to skilled nursing facilities after their hospital stay. This has changed dramatically in the past decade thanks to the availability of thrombectomies (clot-retrieval) that allow specialized teams to remove the clot from your brain.
Telestroke
In addition to these treatments, WakeMed offers an innovative Telestroke program to support stroke patients at hospitals with less medical access, thereby making them stroke capable. The program is a form of telemedicine, providing patients with enhanced in-house stroke care and 24-hour access to stroke neurologists.
Using Telestroke system carts and a two-way live video, audio and image sharing system, consulting stroke neurologists can evaluate a remote patient in real time to diagnose a stroke and determine the best course of action. Patients also receive streamlined access to WakeMed for advanced and post-stroke care.
If you think you or someone you’re with is having a stroke, call 911 and get to your closest emergency department. The faster the treatment, the better the chances for a full recovery and return to normal life.
