Waking Up to the Good Life After Coma — Nigeria McMichael's Story
April 17, 2023
By: WakeMed Health & Hospitals
Categories: Emergency, Physical Therapy, Pulmonology, Raleigh Campus, Stories, Women's
Independence Day is a great time to get together with friends and family, cookout on the grill and watch celebratory fireworks. For Nigeria McMichael, the 2021 event was an especially wonderful time since her family had not been able to get together in 2020 during the height of the COVID-19 pandemic. Loved ones came from across North Carolina and New York to enjoy family festivities on July 4. After the holiday ended, all of Nigeria’s extended family, except her aunt, traveled back to their homes eager for the next holiday gathering.
Losing the After-Party Glow
Days later, on July 8, 2021, Nigeria awoke feeling a little under the weather.
She says, “I noticed the night before that my ankle was swollen, and when I woke up, I felt off, so I told my aunt I was going to get dressed and head to urgent care.”
Nigeria took a shower — with some effort — since she also felt drowsy and sluggish. Afterwards, she went into her bedroom, laid out her clothes and suddenly passed out. Evidently, her aunt heard her body crash to the floor because Nigeria’s next memory was of her aunt holding her head in her arms frantically trying to revive her.
“I felt overheated and looked up at her as she assured me she’d called an ambulance,” recalls Nigeria. “Then members of the fire department entered my bedroom and carried me downstairs. As they were moving me, I passed out again.”
Crushing Cardiac Arrest
Nigeria had gone into cardiac arrest. Emergency medical services workers took turns performing CPR. As one would grow exhausted, a new one would immediately step in. This went on for 45 minutes as they loaded Nigeria into the ambulance and sped her off to WakeMed Raleigh Campus Emergency Department.
Searching for a Diagnosis
Upon arrival to WakeMed, Nigeria was alert. The emergency department care team began asking her check-in questions. She answered their questions but then fell unconscious again. Nigeria experienced three cardiac arrests during this short span.
WakeMed critical care physician Wissam Mansour, MD, was Nigeria’s admitting physician. He immediately ordered computed tomography (CT) imaging with contrast material, so the team could determine a diagnosis. A hollow catheter was inserted through a large blood vessel in her groin for the scan. Critical care physicians James Lakey, MD, and Peter Heetderks, MD, along with several nurses and technicians, supported her during this time.
Nigeria was diagnosed with a pulmonary embolism, which is a blood clot that blocks blood flow to an artery in her lung. This is what caused the cardiac arrests. Her family, including her fiancé, were notified that she would remain in the hospital and require surgery to remove the clot.
Undergoing Lifesaving Surgery
A WakeMed vascular surgeon along with a WakeMed cardiothoracic surgeon performed her procedure. Using an advanced embolectomy catheter, the surgeons removed the large blood clot without the need for an open surgical procedure.
WakeMed’s Pulmonary Embolism Response Team (PERT) was by her side throughout the procedure and recovery. Interventional radiologists, cardiologists, vascular surgeons, intensivists, nurses and pharmacists collaborated to provide the best care possible for Nigeria’s condition.
Healing and Coma
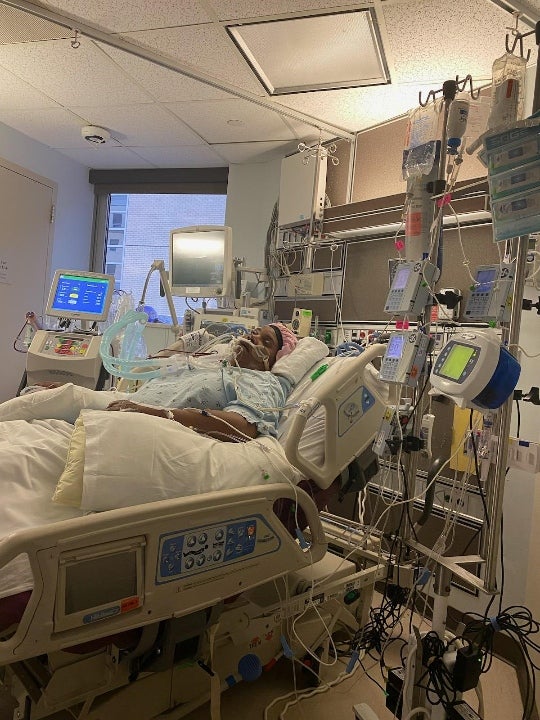
The procedure was a success. Nigeria was then placed in a medically-induced coma in the intensive care unit (ICU) until July 17, 2021.
She explains, “When I woke up, it was a lot to take in. I didn’t know I was on dialysis because everything had shut down. I also wasn’t eating. It took time for everything to come back.”
On July 17, 2021, the team stepped into action to help her navigate back to health. Speech language pathologists Rudi Keene, CCC, SLP, and Whitney Demuro, CCC, SLP, supported Nigeria in feeding and swallowing, so she could start eating. By July 19, several WakeMed physical therapists began coming into her room to help her regain her strength. Just two days later, on July 21, WakeMed dietitian Jessica King, RD, began offering nutritional support. This was all to prepare her for the next step in her recovery: a transition to the WakeMed Rehabilitation Hospital.
Several attending physicians in internal medicine and WakeMed Heart & Vascular continued to monitor Nigeria’s progress leading up to her discharge from ICU. Finally, on July 28, she was deemed well enough for admittance to rehab where she would work with accomplished therapists to regain as much of her independence and mobility as possible before heading home.
Nigeria reflects, “I’m so grateful that my aunt just happened to visit for a few more days. If she had not been there, I would have died. My fiancé would have found me in our bedroom once he returned from work. My 25-year-old son would no longer have a mother.
“And, I can’t say enough good things about the care I received. I think about the EMS workers who administered CPR for nearly an hour. I think about all the providers who cared for me though I was weak, sick and depressed because of what I was going through.”
Going to the WakeMed Rehabilitation Hospital
Nigeria went to rehab physically better but emotionally downcast. She remembers a member of the health care team coming into her room to ask her some questions after she was settled in. Nigeria recalls barely managing the stamina to stay alert — much less answer questions.
Tearing up, Nigeria shares, “I had had a rough day. And, at that point, it was around 9:00 at night. I remember her coming in nicely to ask questions for registration and seeing me there in pain. She patted me on my hand, told me she’d be back later and said I could rest. That meant so much. She saw me. She had a job to do, but she saw me in that state and let me sleep.”
Overcoming Pain and Regaining Strength

The next day, Nigeria met Elizabeth Penny, LRT/CTRS, and Pistachio. Seeing them come in, she felt overwhelmed because she didn’t want to do anything, but Elizabeth willed her to get started.”
“Elizabeth was like a big sister to me, and Pistachio was so gentle. Elizabeth told me I could do it, and she helped me get up. Her spirit was so uplifting.”
Elizabeth also recalls her time with Nigeria.
“I was her rehab recreation therapist. Initially, when she arrived, she was very deconditioned. Her endurance was poor. She had difficulty doing everything from dressing herself, walking, pushing her wheelchair and participating in her three-hour therapy sessions. I turned on some music, and we started moving and laughing. She could just move a little. We had to start somewhere. I incorporated Pistachio into therapy, so she had to work her arms by grooming and brushing him. We used a lot of humor and music to celebrate that she was alive.”
The same day, Nigeria met Julie Gravely who offered her nurturing support.
“Julie helped me get my pants on and washed my hair since I hadn’t washed my hair in two months, you know. She was there for me like a mom. I’ll never forget it,” says Nigeria.
Julie also has fond memories of Nigeria.
“When she came to us in the Rehab Hospital, she was really weak with poor endurance. I was her certified occupational therapist assistant (COTA), and I worked with her every day on activities of daily living skills. We got into a routine of her morning care: shower, dressing, breakfast. Initially, it wore her out just to take a shower. In the therapy gym, we did a lot of different, fun activities focusing on balance, strength and endurance. Slowly but surely, she gained her strength.”
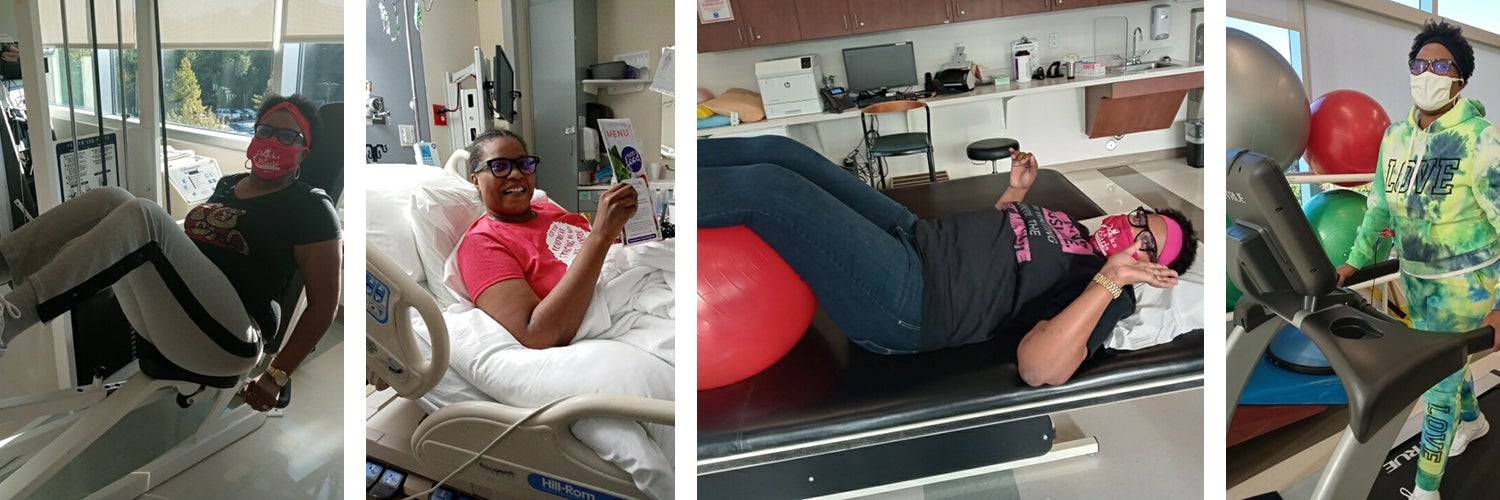
As part of Nigeria’s therapy, the team collaborated to come up with an activity that would prove physically challenging but also fun.
Julie explains, “We did an outing with Elizabeth to Food Lion where she worked and purchased ingredients for her to cook the next day.”
Nigeria was thrilled. She decided to prepare lasagna.
“As a recreation therapist,” explains Elizabeth, “my goal is always to help patients get back to the things they did before. Nigeria worked as a bakery and deli manager at Food Lion prior to coming into the hospital. She was anxious to get stronger and get back to work. She needed to be as independent as possible at home, and she enjoyed cooking. We decided she would cook lasagna. In order to do that, we planned an outing to her Food Lion store to purchase supplies. She had not seen any of her coworkers while in the hospital. We arrived in the WakeMed car. She was able to walk from the car to the front of the Food Lion since she had just started back walking short distances. She sat down in the electric shopping cart. Her coworkers were caught off guard and had no idea she was coming to the store. Tears started flowing from everyone as they observed that Nigeria was doing so well. She was able to pick up ingredients, return to the hospital and make lasagna — taking rest breaks during the process in the transitional living suite in the Rehab Hospital. This is a modified apartment, so patients can practice real life skills.”
Nigeria felt quite accomplished after she prepared the meal, and staff raved about how delicious it was. She had confidence that upon discharge, she would be able to care for herself and also her fiancé who fell critically ill while Nigeria was in the hospital.
Learning Her Fiancé was also Fighting for His Life
Soon after Nigeria went into rehab, her fiancé contracted COVID-19 and was put on a ventilator at WakeMed Raleigh Campus. Oddly enough, he was being cared for in the exact same room in the ICU in which Nigeria endured weeks in a coma. When they took Nigeria to visit him, she was overcome with emotion and grew determined to be as independent as possible once she could return home, so she could care for herself and her fiancé who, too, would be in recovery.
Nigeria remembers, “They wheeled me to the room to see him. I couldn’t believe it. I cried and asked, ‘Is he going to make it?’ They comforted me and wheeled me out of the room.”
Penny recalls this unbelievable misfortune.
“Nigeria was almost at the time of discharge from rehab and about to have her fiancé attend training for discharge. Her fiancé became sick and was put in ICU — the same room that Nigeria had been in. This was even more reason for Nigeria to be independent at home. Her strength was coming back, but she still needed more therapy at home, so she could return to work.”
Celebrating Her Return to Normal

On August 24, 2021, Nigeria was discharged from the WakeMed Rehabilitation Hospital. The team gathered with her to take pictures and show their support. Her son had beautiful shirts made to celebrate her return to health and home. Her aunt was in attendance for that special day as well. Her fiancé was still in the hospital but growing stronger.
While Nigeria was preparing for total independence once she left rehab, WakeMed had prepared at-home support.
“WakeMed Home Health sent nurses to support me daily for a couple of hours. They were so nice,” shares Nigeria. “My aunt also stayed for several more months to take care of me and help me.”

On December 9, 2021 Nigeria and her fiancé were married in a beautiful ceremony. It was an especially emotional time as they both recognized just how much they had to be thankful for: for their love, for their lives.
Looking Forward to Joy Ahead

Today, Nigeria is doing well. She has returned to work at Food Lion, and her son is now expecting his own child. Nigeria is going to be a grandmother, and she cherishes knowing she will be there to celebrate this next step in her son’s life.
Nigeria has never forgotten the amazing team at WakeMed who saved her life. She formed a special bond with Elizabeth and Julie and continues to visit them.

Julies shares, “It is so good to see Nigeria. She looks beautiful and strong! When I was her COTA, I enjoyed every minute I spent with Nigeria.”
Elizabeth shares these feelings.
“Nigeria was always positive and motivated to do anything she could that would help her. Through exercising and finding things she enjoyed, slowly she began to get stronger and stronger. Over the past couple years, she has stopped by to visit and thank us for how much we loved her. Now I take patients to Food Lion where she works, and she encourages them to keep fighting and getting stronger.”
About WakeMed Critical Care
WakeMed features the highest level of critical care services available in Wake County. Our highly trained physicians and staff offer quality specialized care for patients of all ages.
In fact, among our critical care units and services, WakeMed features the highest level Neonatal Intensive Care Unit, the county’s only Neuro Intensive Care Unit and the county’s only Pediatric Intensive Care Unit. These critical care units are supported by board-certified specialty physicians, intensivists, nurses and allied health professionals. If you or your family member has a critical care health need, WakeMed is the place to be.
About WakeMed Emergency Services
The WakeMed system of emergency departments is one of the largest and busiest in North Carolina. As a result, we’ve pretty much seen it all. Our doctors are board certified in emergency medicine, are backed by the highest designated Trauma Center available and bring with them the depth of experience that you would expect from the area’s leader in emergency care.
So, rest assured that no matter where it hurts we’ve got you covered.
About WakeMed Heart & Vascular
WakeMed Heart & Vascular is the leader in cardiac, vascular and thoracic care, using the latest in innovative procedures and treatments for heart and vascular disease. Our caregivers come together to ensure the highest level of quality and compassionate care, which is at the heart of all we do.
Our caregivers are the reason for our continued success. We serve our patients with a quality-driven belief that makes us a leader in successful patient outcomes and heart-warming, family-centered care.
As a cardiovascular patient of WakeMed Heart & Vascular, we put you first and treat you like family.
About WakeMed Home Health
WakeMed Home Health’s team links patients to WakeMed, a world-class hospital system that is at the forefront of medical care. We work directly with the physician, WakeMed resources, patients and family members to develop a plan of care that corresponds with each patient’s needs and lifestyle.
Our goal is to help patients regain their independence and the highest level of function in the comfort of their own home.
WakeMed Home Health is Medicare and Medicaid certified, state licensed and Joint Commission accredited, ensuring the highest quality of care for patients and their families.
About WakeMed Imaging Services
WakeMed Imaging Services is a full-service imaging department offering advanced technology, convenient access and prompt testing and results. As professionals who have a true passion for care and caring, we focus on providing excellent, individualized service to each patient. Additionally, we have been designated a Diagnostic Imaging Center of Excellence by the American College of Radiology, one of the largest and most influential medical associations in the United States.
About the WakeMed Rehabilitation Hospital
Our flagship Rehab Hospital is a 103-bed inpatient rehab facility (IRF) with dedicated units and gyms for children’s/pediatric rehab, spinal cord injury and brain injury. These units are equipped with highly advanced technology to address the specific needs of adults and children in recovery.