Does Your Birth Control Need an Update?
December 1, 2022
By: WakeMed Health & Hospitals
Categories: Women's
Medically reviewed by Marili Witt, MD, FACOG
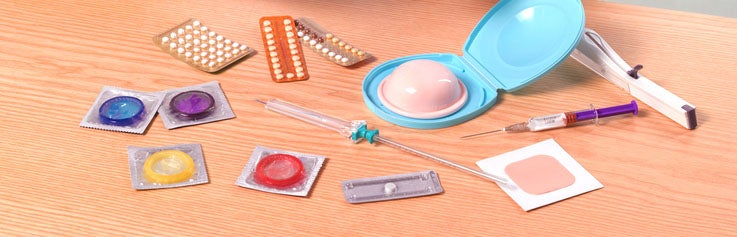
Refresh Your Contraceptive Awareness
Contraceptives are not always about birth control. They are used by many women for many reasons beyond preventing pregnancy: Some women use them to reduce symptoms of PMS or perimenopause, some use them to prevent migraines and some prefer the lighter periods that they have on certain hormone-based contraception.
If you are using birth control products to prevent pregnancy, balancing your contraceptive’s effectiveness with your lifestyle and your physical needs is an important aspect of your health. And it may not stay the same from your 20s to your 40s. Or 50s.
Are you using the same birth control method that you used 10 years ago? Twenty? Over time our lives change and our bodies change. Birth control has also continued to advance and change. It might be time to check in and consider whether your birth control is meeting your current needs. There may also be some new options in the world of contraception since last you looked, and they may be worth your consideration.
Oh, How Types Have Changed
Of course, abstinence is the only birth control that is 100 percent effective. But if you expect to be sexually active, there are a wide range of options for preventing pregnancy — some new favorites, as well as some classic hits.
Condoms
The condom is still the only type of birth control that also protects against many types of sexually transmitted infections (STIs). But as far as preventing pregnancy, condoms are only about 87 percent effective in real use, according to the CDC. If you prefer condoms — say, because you don’t have sex very often or you have more than one partner — you may consider combining condoms with other methods of birth control for greater protection against unplanned pregnancy.
Other Contraceptive Barrier Methods
Condoms are the most effective of all the barrier methods — methods that can prevent sperm from entering the uterus, where they might fertilize an egg. There are a few currently available methods that have waxed and waned in popularity, such as:
- Diaphragm: About 12 percent of women who use diaphragms get pregnant each year, making diaphragms about as effective as condoms when used with spermicide. But if you gain or lose 10 to 15 pounds, you should get refitted for a new diaphragm.
- Cervical cap: A thimble-shaped cup that fits snugly over the cervix, the cervical cap is used the same way as a diaphragm, but its failure rate is higher — about 21 percent.
- Female condom: While they do provide some protection against STIs, female condoms have a failure rate of about 21 percent.
- Sponge: Spermicide-coated sponges, lauded for having a feel similar to vaginal tissue, were taken off the market for a while, but they are back. Don’t celebrate yet, though: About 32 percent of women who have previously had babies and 9 to 16 percent of women who have never had a child will get pregnant each year when using the sponge. The sponge it is also associated with higher rates of vaginal infections.
For all barrier methods, including condoms, one of the main reasons they fail is because they aren’t used exactly as directed. And especially in the heat of the moment, you may not even realize that you are using the product incorrectly.
The Pill, the Ring, the Patch: Combined Hormonal Contraception
Estrogen-containing birth control pills, contraceptive vaginal rings and patches are all are more effective than barrier methods in terms of preventing pregnancy, because they use estrogen and progestin hormones to:
- Disrupt the process of ovulation
- Thicken cervical mucus to block sperm from entering the womb
- Thin the lining of the uterus to prevent implantation of a fertilized egg
These products can be up to 99 percent effective, but they rely on consistent, timely use. Nine out of 100 women will get pregnant each year on the pill because they don’t take it regularly enough. If you have trouble remembering to take your vitamins every day, or to get your oil changed every three months, these methods may be less reliable for you.
Some studies also show that women at higher weights might be more likely to get pregnant while on hormonal contraception than normal-weight women. And some women need to avoid taking estrogen for health reasons — or because hormonal birth control gives them side effects that are hard to tolerate.
Progestin-only Pills (Mini Pills)
These pills contain only progestin — no estrogen — and they work by thickening the cervical mucus so the sperm cannot reach the egg. Progestin pills also thin the lining of your uterus, so menstrual bleeding is lightened. Like other birth control pills, their effectiveness depends on taking the pill at the same time every day, so it has the same 10 percent failure rate as other pills. Its effectiveness can also drop in women at higher weights.
The Shots: Depo-Provera and Nexplanon
These methods are more effective than the pill, patch or ring, and they require less remembering on your part:
- Depo-Provera is a form of the hormone progestin, given as an injection into your buttock or arm. It is taken every three months and is 99 percent effective if you get your injections on time.
- Nexplanon is a single rod of hormone (the size of a matchstick) that is placed under the skin of the upper arm. It delivers progestin over a three-year period. It is almost 100 percent effective — making it one of the most effective available forms of reversible contraception.
These products must be injected or implanted by a trained provider, and you’ll need to plan to get them repeated when they run out. About six out of 100 women on Depo-Provera get pregnant each year because they don’t get their next shot in time.
Intrauterine Devices (IUDs)
These small, flexible T-shaped devices are placed through the cervix into the uterus by a trained provider. There two types:
- Copper IUDs, which can be kept in place 3 – 8 years
- Hormonal IUDs, which contain very low doses of progestin and can be kept in place for three to five years
IUDs are nearly 100 percent effective, they can be removed at any time and some women have an easier time with their periods after receiving an IUD. These factors, combined with their longevity and convenience make IUDs a popular choice for women of many ages. The main downsides are up-front costs, especially for women without insurance. Some women experience pain or cramping during or shortly after insertion. And if you are under 20 years old or use a menstrual cup, you have a slightly increased risk that the IUD will move out of place.
Emergency Contraception
This form of birth control may be used within a short period of time after unprotected sex to prevent successful fertilization and implantation of an egg. There are three main types:
- Over-the-counter pills that must be taken within 72 hours of unprotected sex
- Prescription pills that must be taken within 5 days of unprotected sex
- Copper IUDs, which must be inserted by a health care professional within 5 days of unprotected sex but are 100 percent effective (and can be left in place for 10 years)
Neither the prescription nor the over-the-counter pill will cause miscarriage or otherwise affect an established pregnancy. While these methods can be helpful in unexpected situations, if you find yourself using the pills with any frequency then it’s probably time to consider another method.
What’s not Recommended?
These methods of birth control, when used on their own, have a 20 percent chance of failure or higher — and are much more prone to user error:
- Withdrawal (pullout) method
- Spermicides used on their own
- Rhythm method — natural family planning based on a woman’s unique fertility cycle and abstinence during her most fertile days. Some studies say the rhythm method has a failure rate of 50 percent.
Birth Control by the Numbers
 While every woman is unique, there are a few things that tend to change for many women as they move through their lives.
While every woman is unique, there are a few things that tend to change for many women as they move through their lives.
Teens
According to the American Academy of Pediatrics (AAP), nearly half of high school students in the United States have had sex. And up to 80 percent of pregnancies among 15- to 19-year olds are unintended. To reduce the risk of pregnancy in these teens, AAP recommends long-acting reversible contraceptives, such as IUDs or birth control implants.
Other birth control methods such as the pill, a skin patch or a vaginal ring are effective, but only when they are used on time, without missing a dose. An inserted device is sometimes the best fit for younger women who may be more likely to forget taking their pills.
Your 20s and 30s
IUDs or birth control implants are often a good choice for when you’re in their 20s and 30s, too. They are convenient, they don’t require daily maintenance, and they can be easily removed if you want to get pregnant — they have no permanent effect on fertility.
The birth control pill, shot, skin patch and vaginal ring are also effective options at this point in your life. But you should check in with your doctor if you have certain medical conditions or risk factors. For example, if you’re over the age of 35 and smoke, or if you have a history or high risk of breast cancer, your doctor might advise against estrogen-containing birth control. Estrogen increases your risk for blood clots, heart attack, stroke and hormone-sensitive cancers.
Your 40s
About 75 percent of pregnancies in women over 40 are unplanned, perhaps because after age 40 you may think you’re not going to get pregnant. Not so — while fertility does decline with age, it’s still entirely possible for you to get pregnant in your 40s. And if that’s not going to be a pleasant surprise, or if you’re concerned about the risks associated with pregnancy in older women, don’t quit your birth control just yet.
Choosing between an IUD, a birth control implant or hormonal contraceptives may depend on your health situation and your habits and preferences. Symptoms of perimenopause are sometimes relieved by taking estrogen-containing birth control. However, estrogen-containing birth control can also raise your risk of blood clots, heart attack and stroke. You might choose to avoid estrogen-containing options, especially if you have high blood pressure, a history of smoking, or other risk factors. Talking with your gynecologist can help clear up the best option for you.
The bottom line at this time of life is that, if you’re having sex and don’t want to get pregnant, it’s important to use birth control consistently until after you’ve reached menopause, even if you rarely get your period.
Your 50s
Okay, it’s true, after 50 your chances of getting pregnant are low. But you wouldn’t be the first woman in her 50s to have a surprise baby, either. Your chances of pregnancy don’t go away completely until after you’ve reached menopause, meaning it’s been at least one year since your last period or any bleeding or spotting, however infrequent.
If you’re not through menopause but you’re over 50 and you’d like to stop taking hormonal contraceptives, it may be OK to switch to something with less efficacy, such as a sponge or diaphragm. If you are taking hormonal birth control and you like it, it might be safe to use hormonal birth control until age 55 if you have no health risks.
After Menopause
If you have gone through menopause — no bleeding for 12 months in a row — it is widely agreed that you can stop using contraceptives — at least, for preventing pregnancy. But if you have more than one sex partner, remember that condoms are still a must for both partners to prevent STIs — because an STI doesn’t care how old you are.
If It Ain’t Broke
Ultimately, if you want to avoid pregnancy, the birth control method you choose is the one that you will use.
Not all women need to change the birth control they’ve used happily and successfully for years. If the method you are using really works for you, there may be no reason to switch it. But if your health has changed or your life has changed, it may be a good time to review your birth control options with your gynecologist. She can help you review your medical history and sort through any questions or misconceptions about contraception.
WakeMed Primary Care and OB-GYN Can Help
It’s a good idea to start with your primary care provider for basic birth control needs. Call or schedule an appointment today.
WakeMed OB-GYN providers are happy to help evaluate what kind of contraception is most appropriate for your particular needs.
Learn more about WakeMed Obstetrics and Gynecology, and schedule your appointment at a location convenient to you.
About Marili Witt, MD, FACOG
 Dr. Witt is an OB/GYN with clinical interests in high-risk pregnancies, family planning and contraception, and minimally invasive surgery.
Dr. Witt is an OB/GYN with clinical interests in high-risk pregnancies, family planning and contraception, and minimally invasive surgery.
Dr. Witt joined WakeMed Physician Practices after completing her residency at the University of North Carolina at Chapel Hill. She is strongly committed to the mission of teaching future physicians who are in various stages of their education. She has received several teaching awards from both medical students and residents.
Outside of medicine, she enjoys spending time with her husband and two children. She loves to exercise, particularly running and kickboxing.
Sources:
https://www.healthline.com/health/birth-control/options-every-age?msclk…
https://www.webmd.com/sex/birth-control/birth-control-40s-50s
https://www.health.com/condition/birth-control/birth-control-methods-ev…
https://my.clevelandclinic.org/health/articles/11427-birth-control-opti…
https://www.healthline.com/health/birth-control-iud
https://www.cdc.gov/nchs/products/databriefs/db327.htm
https://www.womens-health-concern.org/help-and-advice/factsheets/contraception-older-woman/
WakeMed Sources:
https://www.wakemed.org/care-and-services/brain-and-spine/stroke-progra…
https://www.wakemed.org/care-and-services/heart-vascular-care/resources…